Posted By Dr. Farah Arshad, Breast Cancer Specialist in Lucknow
Most people want a simple answer to this question. Remove the lump, or remove the whole breast? But the truth is, this decision is never that simple. Most articles tell you what each surgery is. Very few explain how doctors actually choose between them. As Dr. Farah Arshad, Breast Cancer Specialist in Lucknow, explains to her patients — the right surgery depends on many layers, not just the tumor.
What Each Surgery Does
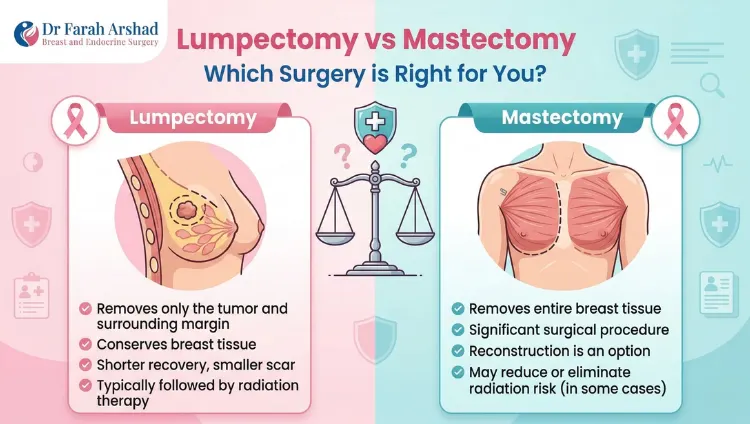
A lumpectomy (also called breast-conserving surgery) removes only the tumor and a small amount of healthy tissue around it. The rest of the breast stays intact. After this surgery, most patients need radiation therapy.
A mastectomy removes the entire breast. Sometimes the nipple, areola, and nearby lymph nodes are removed too. Reconstruction surgery can be done right away or later. Radiation may or may not be needed after.
The important thing most articles mention is this: for early-stage breast cancer, survival rates for lumpectomy plus radiation are similar to mastectomy. That is true. But the real decision goes much deeper than that.
Step 1: The Cancer Type Matters First
Before choosing a surgery, doctors look at what kind of cancer it is. Surgery removes the tumor, but it does not change the cancer’s biology. Here is a simple breakdown:
| Cancer Type | What Surgery Does | What Actually Controls Recurrence |
|---|---|---|
| Hormone receptor positive | Removes tumor | Hormone therapy after surgery |
| HER2 positive | Removes tumor | Targeted drug therapy |
| Triple negative | Removes tumor | Higher recurrence risk regardless of surgery type |
This is why your cancer stage and tumor type must be understood before surgery is even discussed.
The Real Question Doctors Ask
Doctors do not simply ask “lumpectomy vs mastectomy?” They ask: Can we remove the tumor and get clear margins while keeping the breast looking normal? If yes, lumpectomy is possible. If no, mastectomy is likely recommended.
According to Dr. Farah Arshad, a Breast Cancer Specialist in Lucknow, this single question hides enormous complexity—and every patient deserves to understand it before attending a surgical consultation.
What Are Clear Margins and Why Do They Fail?
Clear margins mean no cancer cells were found at the edges of the removed tissue. This is the most important measure of a successful lumpectomy. But margins fail more often than people expect.
Reasons margins can fail:
The tumor was larger than it appeared on the scan. Cancer had spread in tiny amounts not visible on imaging. The patient has dense breast tissue that hides tumor edges. There are multiple tumor sites in the breast.
When margins are not clear, the patient may need a second surgery, a third surgery, or sometimes a full mastectomy. Many blogs do not mention this at all.
Will the Cosmetic Result Really Be Better with Lumpectomy?
Many people assume lumpectomy always looks better. That is not always true.
| Situation | Likely Cosmetic Result |
|---|---|
| Small tumor, large breast | Usually good after lumpectomy |
| Large tumor, small breast | May look worse than mastectomy with reconstruction |
| Tumor near the nipple | Significant shape change likely |
| Multiple tumors | Difficult to preserve normal shape |
Radiation after lumpectomy can also cause the breast tissue to harden, shrink, or become uneven over time. Sometimes mastectomy with reconstruction gives a more balanced result.
The Radiation Commitment Most People Underestimate
Lumpectomy almost always requires radiation after surgery. This usually means daily hospital visits for 3 to 6 weeks. For many patients, this becomes the deciding factor — not the surgery itself.
Patients who live far from a treatment center, are elderly, or have medical conditions that prevent radiation may find mastectomy actually simpler in the long run. Dr. Farah Arshad, Breast Cancer Doctor in Lucknow, notes that for many patients in this region, travel distance to a radiation facility is one of the most practical and often overlooked parts of surgical planning.
When Mastectomy Is the Safer Choice
There are situations where mastectomy is clearly the better option:
Multiple tumors in different parts of the breast (called multicentric disease) make it very hard to remove everything while keeping the breast intact.
A BRCA gene mutation means a much higher lifetime risk of cancer. Many of these patients choose to remove both breasts as a preventive measure.
Prior radiation to the same breast means radiation usually cannot be safely repeated, making lumpectomy less effective.
A large tumor in a small breast may be technically removable but leaves very poor cosmetic results.
What Patients Often Get Wrong About Mastectomy
Many patients believe removing the whole breast eliminates cancer risk. This is only partly true.
| What Mastectomy Does | What Mastectomy Does Not Do |
|---|---|
| Reduces risk of cancer returning in the breast | Prevent cancer from spreading to other parts of the body |
| Removes all breast tissue | Eliminate risk from tumor biology |
| May remove need for radiation | Guarantee cancer will not come back |
The risk of cancer spreading to other organs depends on the tumor’s biology, whether lymph nodes are involved, and the drug treatment given after surgery. Not on whether a lumpectomy or mastectomy was performed. This is one of the most important and least discussed facts in this topic.
Mastectomy and Reconstruction: It Is Not One Simple Surgery
Many articles show mastectomy plus reconstruction as a clean, two-step process. In reality, reconstruction can involve multiple procedures over months or even years.
The process may include placing tissue expanders first to stretch the skin, then an implant exchange, followed by flap surgery using tissue from the abdomen or back, and finally symmetry procedures to match both sides. Possible complications include infection, implant loss, scarring, and the need for revision surgery. It is important to understand this before choosing mastectomy based on the idea that reconstruction is quick or easy.
Follow-Up Care After Each Surgery
After a lumpectomy, patients continue regular mammograms as part of long-term monitoring.
After a mastectomy, routine mammograms are generally not required for the removed breast. Monitoring continues through physical exams and imaging if any symptoms appear.
How Doctors Actually Make This Decision
Here is a simple view of what surgeons consider together before recommending surgery:
| Factor | What Doctors Evaluate |
|---|---|
| Cancer stage | How advanced and widespread is it? |
| Tumor biology | What type and how aggressive? |
| Tumor size vs breast size | Can clear margins realistically be achieved? |
| Number of tumors | One site or multiple areas? |
| Genetic risk | BRCA mutation or family history? |
| Radiation feasibility | Can the patient complete a full course? |
| Patient preference | Emotional comfort, lifestyle, body image |
| Reconstruction options | What is available and realistic? |
Only after going through all of these does a surgical plan take shape.
So Which Surgery Is Better?
Neither is universally better. They solve different problems.
Lumpectomy works best when the tumor can be fully removed with clear margins, the breast shape will be preserved, and the patient can complete radiation therapy.
Mastectomy works best when lumpectomy cannot achieve clean margins, there are multiple tumors, genetic risk is high, radiation is not possible, or the patient wants the lowest possible chance of local recurrence.
Questions to Ask Your Surgeon
Before deciding, ask these directly:
Can clear margins realistically be achieved with lumpectomy? What is the chance I will need a second surgery? Will I definitely need radiation, and for how long? How much will my breast shape change? If a mastectomy is needed, what reconstruction options do I have?
Consult Dr. Farah Arshad — Breast Cancer Specialist in Lucknow
If you or someone you love is facing this decision, getting the right guidance early makes all the difference. Dr. Farah Arshad is a Breast Cancer Surgeon in Lucknow with experience in helping patients understand their surgical options clearly and make decisions that are right for their specific situation — not just what is standard on paper.
The right surgery is the one that fits your specific cancer, your body, and your life. No blog post can make that decision — but the right specialist can walk you through it with clarity and care.